When Diane Flynn’s third child was born with a cleft lip in 2001, her family embarked on a series of six surgeries and appointments with dozens of specialists at Lucile Packard Children’s Hospital Stanford that spanned eight years. For the Flynns, the hospital became a second home.
Diane felt compelled to give back to the hospital that was so supportive of her family, so she became one of five parent leaders of the hospital’s Family Advisory Council, where families provide firsthand feedback on everything from bedside care to food service.
Eight years later, in 2009, the hospital team that was starting to plan for a new children’s facility wanted to gain an understanding of needs from the perspectives of a wider group. They created a design committee that included architects, hospital staff, board members, faculty, and members of the Family Advisory Council.
“About 10 years ago, before the design team or architects had plans, they had parents,” says Diane, who joined the committee as her son, Matthew, now 16, was spending less time in treatment. She wanted to be a voice for families like hers.
The committee’s meetings became open forums for input and brainstorming about what they wanted to see in the new campus. “It didn’t take long for us all to agree—a restorative space that felt light, healing, engaging,” Diane says.
That feedback is present in nearly every aspect of the new Main building, which opened to patients on December 9, 2017. The building combines the most advanced medical tools with a holistic approach to healing—focusing on the family at the heart of patient care.
The concept is reminiscent of Lucile Salter Packard’s founding vision for the hospital: to nurture the body and soul of every child. She recognized the power of nature as an important part of healing. She wanted kids to be treated like kids—not just patients. And she believed that caring for a child involved the whole family.
Feelings Matter
There is deep evidence that a hospital’s physical environment and the well-being of patients and families are closely related. In 1984, two years before planning for the original Packard Children’s Hospital began, Science published a study by environmental psychologist Roger Ulrich, PhD, that was lauded as the first to use modern medical research to support the healing effects of nature.
“By the early 1980s, evidence supporting the stress-reducing effects of nature was so consistent, and we understood that natural beauty’s effects were much more than skin deep,” Ulrich says. Now, he explains, it is routine for hospitals to be built to support a positive psychological experience for patients, but he points to the original Lucile Packard Children’s Hospital as an early adopter when it opened in 1991 with terraces on each floor and a garden at the center.
The new Main building, which is connected to the original (West) building, takes a similar approach by challenging the fundamental mindset of being inside a hospital, beginning with the experience of a patient arriving there.
“A common issue in health care is that traditional hospital design places operating rooms and imaging services on sub-ground level floors to accommodate heavy surgical and diagnostic equipment,” says Robin Guenther of Perkins+Will, lead architect. Perkins+Will collaborated with Hammel, Green and Abrahamson Architects, Inc. on the project. But the practice of moving patients down into a basement level, she explains, can exacerbate feelings of fear or anxiety that children experience prior to “scary procedures” such as surgery.
Reflecting a shift away from this, the new hospital’s pedestrian entrance is at ground level, which is also the location of the treatment center (surgery, interventional services, imaging, and nuclear medicine). Families don’t have to traverse below ground and instead enter the main lobby and have only a few choices about where to go next: up the staircase or elevator, or across the lobby into the surgery and imaging unit.
“From a patient experience perspective, it is revolutionary,” Guenther says.
As visitors move through the building, elements of Northern California’s native environment provide a sense of being alongside nature, despite being in a hospital.
Outside, three and a half acres of gardens and green space surround the building, and inside, waiting areas have large picture windows. Each patient room has a planter box outside the window and a view to the gardens. Glass doors in the new Harvest Café open to an outdoor dining patio over-looking the Dunlevie Garden, which has native plants and animal installations that represent California’s eco-regions, including a puma den, a gopher’s burrow, and a redwood tree fort.
And most uniquely, each of the building’s four patient care levels has two outdoor decks—one for patients and visitors, and one for staff—ensuring easy access to restorative spaces and to nature.
The hospital’s use of natural light and holistic approach to healing are also embodied in the Sanctuary, which includes a private prayer chapel and access to a meditative labyrinth.
As the new Sanctuary was conceptualized, the team again called on the Family Advisory Council, whose members represent a variety of faiths (and non-faith), to build something that would appeal to many spiritual beliefs and backgrounds. The result “is a space that is multicultural, multidimensional, and goes beyond religious practice,” Guenther says. “It is about recognizing that we are whole people who have physical bodies, minds, and a spirit and we need to provide a place for people to keep in touch with that.”
Sweating the Small Stuff
The 149 new patient rooms, nearly all private, serve as the center of a child’s hospital experience, not just a place for medical equipment and visits from clinicians.
The healing, comfortable, and spacious rooms, designed for the whole family, serve as home base for mealtimes, movies, and games and include sleeping accommodations for two family members.
“When a parent can have a private room, their own space with their child, they can create a quiet and healing space,” says Karen Wayman, director of the Family Advisory Council. “That’s so important for a parent’s relationship with their child.”
To refine the rooms, full-scale detailed mockups were constructed in a warehouse. Everything was in place, including medical equipment, patient beds, sinks, televisions, light switches, outlets, and hand sanitizer dispensers. Then representatives from the full care team of physicians, nurses, and parents walked through to share feedback.
“We reviewed bedside tables, laid in different sleeper beds, tested the comfort of rocking chairs, examined the distance from the couch to the patient’s bed, to the television, and to the phone charger built into the wall,” Diane says. “Everyone had a different perspective. For me, the lighting was really important. When my son was in the hospital, I didn’t want to disturb him by turning on the overhead lighting to read, so for the new building the design committee made sure we would have cozy reading lights in each room.”
Parents also championed having bathtubs in many of the bathrooms instead of standing showers to make bath time easier for little ones. Their input also resulted in the inclusion of a family lounge, laundry facilities, and a family kitchen on every patient floor to help families maintain day-to-day routines. “You just don’t think about it until you walk it from a patient or parent perspective,” Diane says.
The collaboration between providers and parents was key. “Providers learned about the parents’ experiences in the hospital, and parents had an opportunity to see how things worked from the provider prospective,” Wayman says. “Both sides of the equation were critical to creating a healing space.”
Stimulating the Mind, Restoring the Body
Finally, priority was placed on family being able to connect the worlds of learning and healing, mind and body, resulting in abundant access to nature, art installations, play spaces, and other interactive elements.
“You’re always trying to engage your child in something when you’re in the hospital. When my son had to fast before his surgeries, we would walk the halls to try to keep his mind off his hunger,” Diane says. “We’d stop at the art on the walls and play ‘can you find’ games. Bringing in art and other elements of interactive play like this to the new hospital was crucial.”
Opportunities to learn about the local environment and nature themes are prominent across the campus. Visitors can follow animal footprints and learn about the state’s diverse wildlife. The main elevator is built to look like a tree growing through the center of the building, clad in reclaimed redwood from the deconstructed Moffett Field hangar in Mountain View, California.
California’s ecosystems are also part of the visual wayfinding system that helps direct people through the building. Stanford University ecologists and Packard Children’s patients helped select two animal “ambassadors” native to each floor’s eco-region. Patients and siblings also helped select interactive play structures for the hospital’s gardens and large animal structures that serve as directional landmarks on each floor. “This is a Northern California hospital in a place where people value preservation of species and nature. It was important to create a building that exhibited stewardship of those values,” Guenther says.
But an element of whimsy fit for children remains. At first, a life-size sculpture of a pair of hadrosaurs—the only known dinosaurs to live in Northern California—worried parents on the design committee. “We were concerned that a dinosaur would be scary to little kids,” Diane recalls. So now, the dinosaurs are wearing bunny slippers to make them look more friendly.
Indoor playrooms on each floor, designated by age group, provide spaces for arts and crafts, group games, and other activities that involve the whole family.
“There is endless evidence that supports the medical need for healing elements in the hospital. But at the end of the day, what makes it work is that it feels very human. What we wanted was an expansion of Lucile Packard’s original vision that would not lose the charm and the humanity of the original,” Guenther says.
“As a parent who has had a sick child, any time you step foot into a hospital it brings back a rush of emotions, some good, some challenging,” Diane reflects. “For me, despite the difficult memories, I always had this feeling that the hospital was a pleasant place to be, and I tend to get filled with overwhelming gratitude for that. I keep envisioning my son in the new space at 2 and 3 years old. He would have absolutely loved the new garden, the sculptures, the opportunity for exploration.”
Wayman echoes that: “Parents bring the lived experience with them. They’ve walked the walk with their children. While care teams’ lived experience is providing care and they have an invaluable perspective on the safety and efficiency of the new design, families look at it with heart. And no one else can do that.”
At a Glance: Advanced Technology
Innovative medical technologies make care more efficient and effective for children. They include:
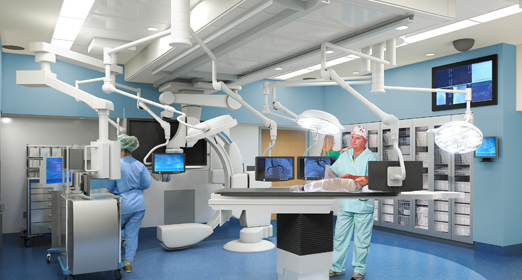
Six new surgical suites, including a neuro-hybrid surgery suite that combines diagnostic imaging services within an operating room. Rather than having to keep patients anesthetized and transport them to another location for a scan, the technology is all in one location. Surgeons can scan the patient and see right away if they’ve successfully removed a tumor, and patients will be able to heal faster.
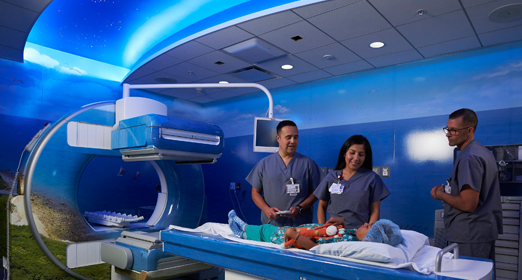
One of the nation’s only standalone combined PET/MRI scanners dedicated to pediatric patients. The machine, designed in part by Stanford engineers, measures how patients’ tissues and organs are functioning to understand how diseases are behaving in their bodies. It provides less radiation exposure and is smaller and less invasive than equipment used for adults, which makes imaging faster and more comfortable for children.
This article originally appeared in the Winter 2017/2018 issue of Packard Children’s News.
Reprinted with permission from Stanford Medicine magazine.
Photographs by Steve Babuljak, Leslie Williamson, and Toni Bird.