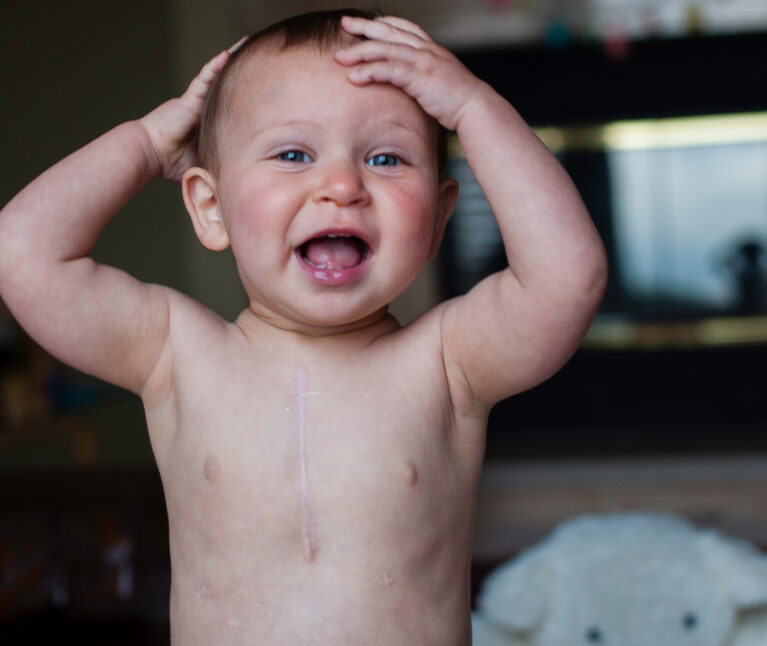
Meet Elena
Though many pregnant women rush to the hospital during labor, few arrive as Tara Sharp did, flying 90 miles by emergency helicopter from Sebastopol to Palo Alto. Her doctors at Lucile Packard Children’s Hospital, who already knew of her baby’s rare heart defect through prenatal diagnosis, were ready for her arrival.
“As soon as we got to Stanford, I felt relieved,” says Tara. She hadn’t expected to go into labor three weeks early. But she had planned to deliver at Packard Children’s, where pediatric cardiovascular surgeon Frank Hanley, MD, would rapidly assess whether her baby would require heart surgery. “We’re in the best hands possible,” she recalls thinking. “This is out of my control now.”
Family History
Tara’s journey to Packard began with unexpected sonogram results. “The doctor said, ‘There’s something wrong with your baby’s heart, and we don’t know if she’ll survive.’” Tara says.
Six months pregnant, Tara and her husband, Ben, were eagerly awaiting their second child. Now, instead of telling their older daughter to expect a sister, they wondered if their baby would live.
A genetic counselor asked about the family history of heart problems. One aunt, Tara learned from her mother, had a mild version of tetralogy of Fallot, the defect detected in a severe form on her own baby’s sonogram. Then Tara’s mom, Heather, revealed something else: More than 50 babies on her family tree, including one of Heather’s own siblings, had died in infancy due to severe versions of the same heart defect. It was the first Tara had heard of this aspect of her family’s past.
But Tara’s pediatric cardiologist in Santa Rosa offered hope. “She told us the best surgeon in the world for tetralogy of Fallot is Dr. Hanley, and that he practices right here at Packard Children’s,” she says.
She smiles, remembering her relief. “We were glad to know Dr. Hanley happened to create the surgery for this particular condition.”
Hanley, who directs the Children’s Heart Center at Packard Children’s, invented a surgical repair called unifocalization that has helped hundreds of children overcome complex tetralogy of Fallot. The defect is composed of several structural abnormalities in and around the heart, including a missing or malformed pulmonary artery that carries blood to the lungs. To compensate, the body develops small “collateral” arteries that travel from the aorta to the lungs. This abnormal anatomy increases blood pressure and causes lung damage. The defect also prevents the body from receiving fully oxygenated blood. Without surgical repair, most patients die in infancy or childhood.
Hanley advised Tara to deliver the baby, who would be named Elena, at Packard Children’s.
“We wouldn’t know the details of Elena’s collateral blood vessels until she was born and could received cardiac catheterization,” says Hanley, who is also the Lawrence Crowley, MD, Professor of Child Health at Stanford School of Medicine. “Most infants with this condition don’t require newborn surgery, but about 10 percent do. So we wanted to assess Elena’s condition quickly.”
Coordinated Care
Tara was referred to the Center for Fetal and Maternal Health at Packard Children’s, where patient care coordinator and genetic counselor Meg Homeyer helped navigate her remaining prenatal care, including diagnostic and consultative appointment with numerous specialists. “Such a multidisciplinary group of people need to be involved in these complex cases, so we try to do everything we can to make the process less difficult,” Homeyer says, noting that some of Tara’s monitoring was performed in Santa Rosa to save her from making extra trips to Palo Alto. “We want the patient’s experience to be as simple, understandable, and empathetic as possible.”
“Having someone like Meg helped give us a center,” says Tara, who was scheduled to have a cesarean section shortly before her due date. Instead, she went into labor three weeks early.
“From the moment that Tara went into labor, throughout the process, every step of the way, someone clearly laid out what might happen, what our choices were, and what the consequences may be,” Ben recalls. “I can’t imagine a better care and better support than we had. There was an incredible, unusual compassion that I don’t know how you pay back.”
Surgery and Recovery
Elena’s birth went smoothly, but her days were not easy. “It was touch and go,” Tara says. “It was a full week before we knew she could breathe on her own, before the doctors were able to perform the catheterization, and realized they could postpone surgery.
After 12 days in the neonatal intensive care unit, Tara and Ben were excited to take Elena home to big sister Cecilia.
For patients with tetralogy of Fallot who do not need surgery as newborns, it’s better to wait a few months to fix their hearts, Hanley explains, since the unifocalizaiton surgery is so technically extensive and involves trauma inside the chest. But waiting carries the risk of overexposing the lungs to dangerously high blood pressure. To strike a balance, most unifocalization surgeries are performed at a few months of age. Elena returned to Packard Children’s for surgery when she was almost 6 months old.
In the operating room, Hanley located all the collateral arteries that were carrying blood to Elena’s lungs and used them to construct a new pulmonary artery.
“It’s like rebuilding the trunk of an oak tree from branches scattered around a field,” he says. Hanley replaced an abnormal heart valve and closed a defect between the right and left sides of Elena’s heart, testing the blood flow through the new artery to make sure it would adequately supply her lungs.
Few surgeons in the world attempt the marathon procedure, which takes about 10 hours. For Hanley, it was almost routine.
“Families come to Packard Children’s from all over the world because of our focus on the management of this congenital heart problem,” Hanley says. “Elena’s case wasn’t the simplest unifocalization I’ve performed, but not the most complex either.”
But for Elena’s parents, it was the most important operation Hanley had ever done. After the surgery, Tara says, “Dr. Hanley appeared out of thin air, very calm, and said everything was as expected. My husband and I just held onto each other.” The heartfelt, “thank you” they offered him didn’t seem like enough, she adds. “How do you thank the person who saved your child’s life?”
Following the surgery, Elena recovered in the cardiovascular intensive care unit under the watch of Loren Sacks, MD, a pediatric critical care fellow. Fellowships, many of which are funded through philanthropy, support education and training for future leaders of pediatric medicine.
“The opportunity to come here and learn from these physicians wouldn’t be possible without the generous gifts that have been given to this institution,” Sacks says. In working with the Sharp family, Sacks experienced firsthand the transformative power of Packard’s exceptional care. As he sat with Tara at Elena’s bedside, he recalls, Tara shared a startling realization.
“Tara told me it had just hit her that Elena would be the first member of their family expected to survive this disease,” Sacks says. “I choked up. It was amazing to be part of giving this to the family, especially in light of how afflicted they had been across generations.”
Healthy and Content
Elena, now 15 months old, is not yet aware of her significant place in family history. Healthy and content, she’s focused on walking, giggling, and chewing on everything with her new teeth. After her difficult first year, she’ll grow up enjoying typical childhood activities.
“She’ll be able to play on the playground, run around the neighborhood, and ride bikes like all little kids do,” Hanley says.
Meanwhile, the genetic counseling team at Packard Children’s is still investigating the genetic bassis of her heart defect. It they’re able to identify the genes involved, Elena’s case might shed light on the origin of tetralogy of Fallot in other families, too.
“Had Elena been born even 15 years ago, she likely wouldn’t have survived,” Tara says. “Packard Children’s has changed our family forever. Looking at her, you would never know that anything had been wrong.”